3 Questions: Mriganka Sur on the research origins treating Rett syndrome
On March 10 the FDA approved Trofinetide, a drug based on the protein IGF-1; the MIT professor’s original research showing that IGF-1 could treat Rett was published in 2009
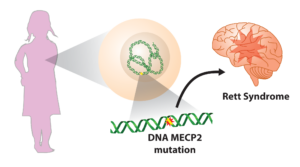
Mutation of the MECP2 gene on the X chromosome causes Rett syndrome, a severe neurodevelopmental disorder. Illustration: Tom DiCesare
Rett syndrome is a devastating developmental disorder, principally occurring in girls, caused by mutations in the gene MECP2 that leads to severe cognitive, motor, and other symptoms. As such, the March 10 approval by the U.S. Food and Drug Administration of the first-ever treatment for the disorder, a drug called Trofinetide based on the natural protein IGF-1, brings new hope to patients and their families.
The approval is also a dream come true for Mriganka Sur, Paul E. and Lilah Newton Professor of Neuroscience in The Picower Institute for Learning and Memory and the Department of Brain and Cognitive Sciences at MIT. His lab’s preclinical discoveries in mice, particularly a highly influential paper published in 2009, provided the first demonstration that injecting IGF-1 or its peptide fragment could reverse the effects of reduced or altered MECP2. This provided a mechanism-based rationale for IGF-1 as a potential therapeutic intervention. And Sur’s lab has never stopped studying Rett syndrome since.
The research began nearly 20 years ago when his lab was studying a famous phenomenon in neuroscience: When an animal’s eye is blocked during a critical period of development, the brain shifts neural connections called synapses to devote more brain power to the unblocked eye. Sur’s lab investigated the molecules involved in this flexibility, or “ocular dominance plasticity,” and discovered IGF-1’s role. Here, Sur discusses his Rett syndrome research.
Q: How did your lab discover that IGF-1 might be a potential Rett syndrome therapeutic?
A: We decided to study the molecular basis of ocular dominance plasticity using a large-scale, unbiased screen. An interesting gene set that changed when an eye was closed was the IGF-1 gene set named for the growth factor IGF-1. When we checked one week after closing the eye, a binding protein for IGF-1 had gone up. It soaked up a lot of IGF-1. That suggested that to make connections change you must decrease molecules like IGF-1.
This was published in a paper in 2006 in Nature Neuroscience, where Daniela Tropea, who was a postdoc in the lab, led the experiments. The icing on the cake was when Daniela delivered a peptide form of IGF-1 to the brain. When she did that and closed the eye, thereby overcoming the reduction of IGF-1, then this shift of synapses did not happen. The addition of IGF-1 into the brain stabilized synapses and made them resistant to change, essentially making them adult-like.
In 2007 the lab of Adrian Bird in Edinburgh made a mouse line in which they could keep MECP2 in check for the first five or six weeks of life, so that the mice began to develop Rett syndrome-like symptoms. But then Adrian’s lab turned the gene back on and the mice largely recovered. I was immediately struck by this discovery. It showed that Rett syndrome is not a disorder of degeneration, it is a disorder of aberrant and even abnormally prolonged development: loss of MECP2 likely reduces molecules that the brain requires for normal development, but adding back these molecules could enable the brain to develop normally, at least to some extent.
The developing brain shows pronounced plasticity, as demonstrated by ocular dominance plasticity in the visual cortex. This plasticity occurs only during early life, and not later. If mice missing MECP2 had aberrantly prolonged development, they should show this plasticity later in life as well. Daniela and I decided to do an experiment to test this idea. We asked whether we could use our visual cortex paradigm to ask, is there prolonged plasticity into adulthood in Rett model mice and can we reverse it by adding IGF-1? We did this using Rett model mice from the lab of Rudolf Jaenisch at the Whitehead Institute for Biomedical Research.
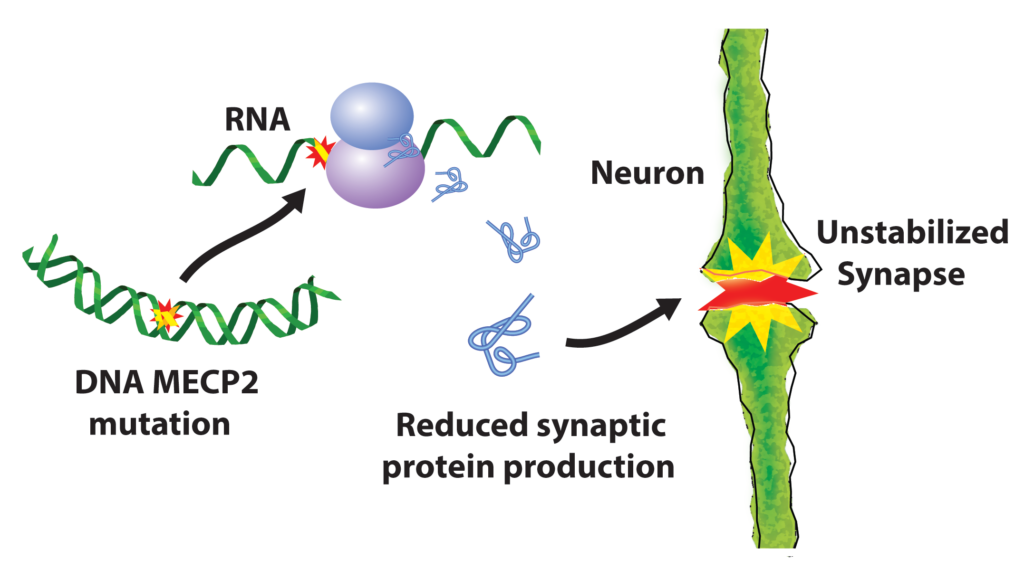
Unlike in normal mice, where there is only a critical time window of plasticity in the visual cortex, Rett model mice showed an effect of closing one eye even in adulthood. We immediately then asked, is there reduced IGF-1 in the brain? And there was, and there was increased IGF-1 binding protein. These mice were in a state of perpetual plasticity.
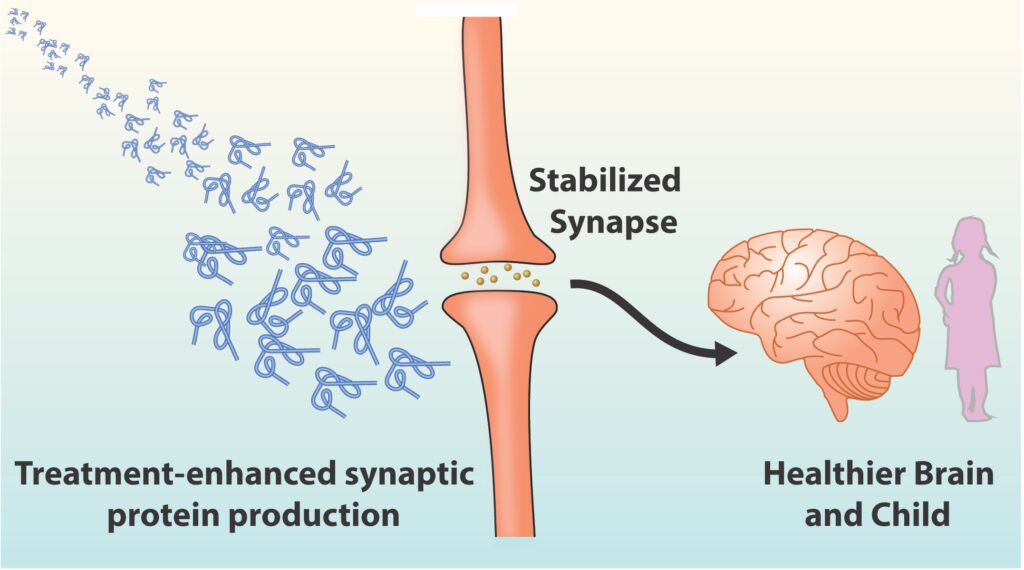
We reasoned if we could give adult Rett model mice a peptide form of IGF-1 via injection the effect of this perpetual plasticity should go away, meaning that the animals should not show an effect of the eye being closed — as occurs when mice normally mature. And that’s what happened. We showed that IGF-1 peptide increased expression of a number of synaptic molecules and made excitatory synapses stronger. This provided a powerful mechanism for explaining the effects of the drug. Finally, we asked, do the mice do better in other ways? We found that the mice lived longer, that they moved better, and other symptoms improved.
We published that discovery in 2009 in PNAS: In a mouse model we showed that by understanding the molecules underlying Rett syndrome’s prolonged development and plasticity we could intervene to potentially offset the molecular and synaptic deficits and treat the disorder. This is the foundational discovery behind Trofinetide and its mechanism of action in Rett syndrome.

Q: Tell us about your lab’s continued work on fundamental mechanisms of Rett Syndrome?
A: We’ve never stopped working on Rett syndrome. It’s a devastating disorder, and there is certainly still much left to learn. In 2014 we published another paper in PNAS showing that doses of recombinant human IGF-1 were effective in mice. And I was also the co-author in that same journal later that year showing encouraging results in a small human clinical trial.
We’ve also done more research, right up to the present day, to understand the fundamental mechanisms of how the genetic mutations perturb brain development. In 2017 using induced stem cell cultures derived from patients and normal subjects, we found that when MECP2 is lacking, microRNAs critical to proper brain development become misregulated. Overexpression of the microRNAs prevented new neurons from being born, whereas inhibiting the microRNAs enabled healthy neural birth. This was a surprisingly early effect of Rett syndrome that we demonstrated directly in human neurons and their progenitors.
Last year we used an innovative combination of advanced imaging methods and human stem cell-derived organoids to show that in Rett syndrome, the migration of neurons to the cerebral cortex becomes much slower and highly erratic. These discoveries led to the sobering realization that there can be very early changes in brain development due to the genetic mutations of Rett syndrome.
Q: What is the significance of seeing this basic research achieve clinical utility and impact?
A: By studying plasticity in normal mice and the fundamental mechanisms by which synapses change, and hence change brain function and behavior, we moved into analyzing the effect of a gene that underlies a devastating brain disorder. IGF-1 peptide has become the very first molecule to reach this stage for any developmental brain disorder in that it is a mechanism-based therapeutic. Based on an animal model and doing the mechanistic analysis of why does the gene affect the brain and how might we offset it, we set the course for the first drug to treat Rett syndrome.
A lot of the early work was Daniela’s insight in terms of how to think about basic mechanisms of developmental plasticity and apply them to brain disorders. This was completely uncharted territory as to whether plasticity would be a phenomenon underlying developmental disorders, and whether the visual cortex in the mouse could then model the disorder. And finally, we had the idea that a molecule that has a role in regulating this plasticity can be applied to the disorder. Many ideas in science don’t work out, but this one did. Several people from my lab participated in the discovery. We also could not have tested these ideas without our collaboration with Rudolf Jaenisch and his lab. He was very generous with his lab’s resources — we had no grant funds for this work at that time — and our labs have now collaborated on several studies since then.
It is the dream of every neuroscientist to have an impact on the world in some way. And this is my dream come true!
David Orenstein | Picower Institute for Learning and Memory
This article first appeared in MIT News on March 13, 2023.